by: Doris Ma
Sleep patterns could be the key to predicting one’s likelihood of developing Alzheimer’s disease (AD). A recent study published in JNeurosci shows that the accumulation of β-amyloid and tau proteins are associated with the disease which could be an early indicator of AD.
Two proteins are thought to be the culprits of cognitive deterioration leading to AD: Tau proteins and β-amyloids. Tau proteins are markers of brain injury that spill into cerebrospinal fluid (CSF) through the breakdown of cellular membranes leading to cell degeneration and cell loss, while β-amyloid (Aβ) are amino acids that are found to be the main deposits in amyloid plaques found in AD patients.
Sleep spindles and slow oscillations are characteristic of electroencephalographic (EEG) rhythms during slow-wave sleep (SWS), the deepest phase of non-rapid eye movement (NREM) sleep, which is considered crucial to memory formation and synaptic plasticity. Sleep spindles are bursts of brain activity that occur to inhibit mental processing and promote a tranquil state where the person can progress to the next stage of deep sleep. On the other hand, slow oscillations are slow frequencies (≤ 1 Hz) in the corticothalamocortical network, which represents neurons activating and deactivating in synchrony during slow-wave sleep and deep anesthesia, otherwise considered as the default rhythm of neural activity.
The coupling of slow oscillations and sleep spindles in SWS reactions promote memory consolidation in adults. Hence, the disruption of these coupled reactions eventually leads to the disruption of the brain’s ability to communicate with other cells, causing the most apparent symptoms of AD: memory loss. Recent studies on rats and mice suggest that there may be associations between sleep waves, tau, and Aβ proteins.
The decrease in sleep spindles is a good indicator of Tau pathology because they are affected by sleep/wake regulating centers that usually decline with age. They are also associated with sleep-dependent motor learning and memory. Thus, a decrease in these neuroplasticity-promoting processes could cause an individual to be more vulnerable to the buildup of Tau pathology. Using these indicators, scientists can have a better idea of a time-sensitive window to measure biomarkers which could predict one’s susceptibility to AD.
Researchers from UC Berkeley and UC Irvine used three methods to predict the AD pathology in male and female older adults: PET measures of Aβ and tau, EEG sleep recordings, and retrospective sleep evaluations.
PET Imaging Analysis
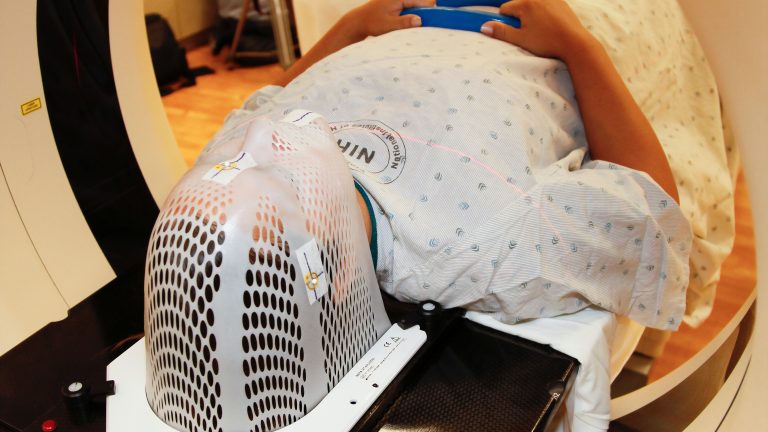
Researchers recruited 101 cognitively normal older adults from the Berkeley Aging Cohort Study to conduct a longitudinal study of cognitive aging. The participants were enrolled in positron-emission tomography (PET) and magnetic resonance imaging (MRI) data collection. PET imaging is a medical technology that measures metabolism in the body, in which researchers use to measure tau and Aβ pathology in older adults. On the other hand, MRI uses strong magnetic resonance to create detailed images of the brain. All participants were free of depressive symptoms and were not on antidepressants or hypnotic medications that may affect brain activity, and all displayed normal performance on neuropsychological testing.
Sleep EEG Analysis
Thirty-one subjects then completed sleep EEG assessment using a test called polysomnography by Grass Technologies systems. A sleep score was then developed using standard criteria by a single trained scorer blind to PET data. Sleep quality measures including total sleep time, wake after sleep onset, sleep efficiency, arousals and respiratory events were scored following American Academy of Sleep Medicine guidelines. The EEG data was also decomposed using the researchers’ published DETOKS method, classifying spindles as fast (13-16 Hz) or slow (11-13 Hz).
Sleep Questionnaire Analysis
Ninety-five subjects wore a wrist-based actigraph on their less dominant hand for seven days. The actigraph collects information about gross motor activity in order to monitor human rest/activity cycles. The subjects also completed a questionnaire about lifespan sleep duration and sleep quality change to confirm actigraphy data. A percent sleep duration change by decade and sleep duration slope graph was generated.
Statistical Analysis
Lastly, researchers used t-tests to assess differences in sleep EEG measures and PET-defined groups. SO-spindle coupling differentiated 2 tau groups, so individuals with categorically high medial temporal lobe (MTL) tau had significantly lower SO-spindle coupling than individuals with categorically low MTL tau burden.
Results
The growing interest in the preclinical stage of AD has sparked research in the field, allowing researchers to realize the shifting role of sleep in relation to AD. Researchers found that individuals with higher MTL Tau were associated with significantly weaker SO-spindle coupling, and those with lower MTL Tau had stronger SO-spindle coupling, confirming that disruptions to non-REM SO-coupling is associated with high MTL tau burden. SWA disruption was also confirmed to have a more significant effect on cortical Aβ than on MTL Tau. The results from the sleep questionnaires also show that a decrease in sleep quantity throughout aging, from the 50s through 70s, was associated with higher levels of β-amyloid and tau later in life.
This research proposes that changes in brain activity during sleep and sleep quantity during specific time frames could serve as a warning sign for AD, allowing for early preventive care. Lead researcher Joseph R. Winer from UC Berkeley shared that the next steps of this project is to investigate people’s sleep/wake cycles in their own homes rather than in a lab setting, in order to more intricately understand the applications of this knowledge. The ultimate goal of this project, he says, is to be able to “intervene at some point in people’s lives and improve people’s sleep to hopefully slow the progression of disease.”
Image Credit: Unsplash